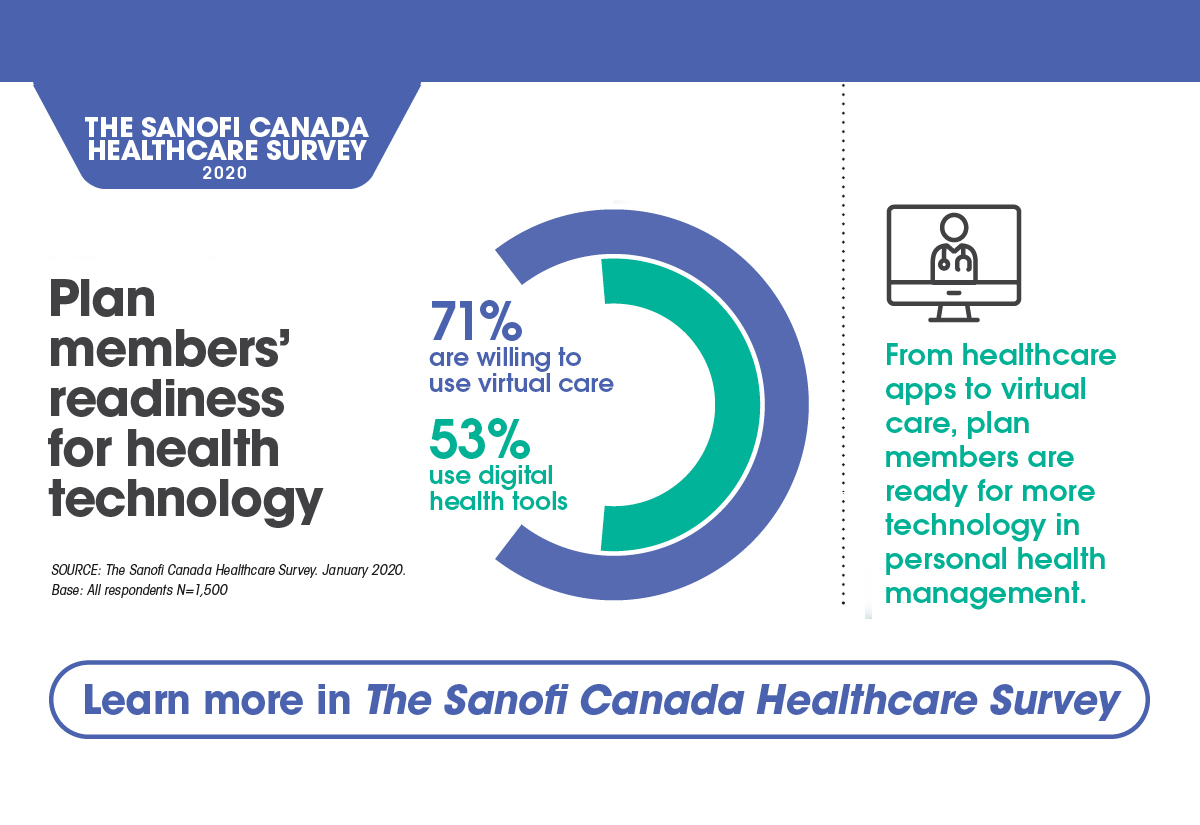
With limited access to in-person healthcare for such a long time, healthcare plan members have become used to technology and better health management with advanced tech. Virtual care, where physicians can diagnose, treat, and monitor patients remotely, has been a welcome addition to personal health management.
Throughout the pandemic, long wait times or no availability for appointments were the norms. With so many roadblocks, virtual care became the preferred choice. In fact, the 2021 Sanofi survey indicates that virtual care has become a standard offering for benefit plans. With the use of healthcare apps that patients now rely on for cross-monitoring with their healthcare practitioners, plan members want more options added to the healthcare tech market.
Supporting the shift in healthcare technology
There are major concerns from plan members returning to the workplace due to lax public health safety measures, working with individuals that could transmit COVID-19 or some other disease, and time lost due to the commute. As virtual health care continues to be prevalent in how plans are administered, members want additional benefits like wellness and personal spending accounts that will help with physical fitness programs and more access to online mental health resources.
The demand for increased virtual healthcare services continues to grow. New applications that allow real-time chat or text with practitioners is no longer an option, but a necessity. The benefit of providing access to virtual healthcare tech and its benefits is recognized by employers because when employees have what they need, they will be more positive when working, which results in avoiding lost time or productivity.
Wellness for the future
Since 86% of plan members place a huge emphasis on developing a wellness culture, this must be integrated into the company culture and benefits plan. Adding a wellness component to the plan helps in keeping and retaining the best talent, addressing stress-related issues, and promoting a relaxed workplace that gets things done.
According to the Sanofi survey:
- 55% of plan sponsors are anticipating challenges in health and wellness stemming from a hybrid workforce model. In all the challenges named, mental health was at the core of each one
- 68% of employees have stress and isolation issues when working entirely from home
- 65% get anxious wondering if their co-workers have been vaccinated
Crafting an effective wellness culture takes time and patience. Using a health and wellness engagement survey that addresses the different types of programs needed can speed up the process of developing something tangible for plan members. While plan sponsors understand the members want physical fitness and wellness at the forefront, only 67% of plan sponsors are planning to invest in wellness outside of the current health benefits plans within the next three years. This figure is down from 75% in 2020. Additionally, the push toward more mental health services indicates that other areas like wellness and physical fitness may suffer.
The hybrid work model may be the current situation, but the chance of things moving back to a fully virtual environment is great. With the impact of COVID-19, 93% of plan members want to continue working from home, and 57% want to work from home on average. This supports plan sponsors who want 45% of their employees to work from home at least part-time.
Wellness and physical fitness benefits can be designed for plan members to use apps that help them work out, monitor their health, and more. The better they feel, the more productive they are and the better they sleep at night. History shows that companies with great wellness cultures do better overall. With plan members continuously pushing for wellness programs that positively affect them, it’s time to close the gap and move deeper into healthcare technology.
People Corporation can assist in getting your health technology set up for now and in the future. For more information, contact us today!
Written by Brendan Hickey, Director, Health Solutions at People Corporation, with insight provided by Shannon Darvill, Consultant at Silverberg Group, a People Corporation Company, and a Sanofi Canada Healthcare Survey Advisory Board Member.
[i] https://www.benefitscanada.com/news/bencan/canadians-cite-91-satisfaction-rate-with-virtual-health-care-survey/